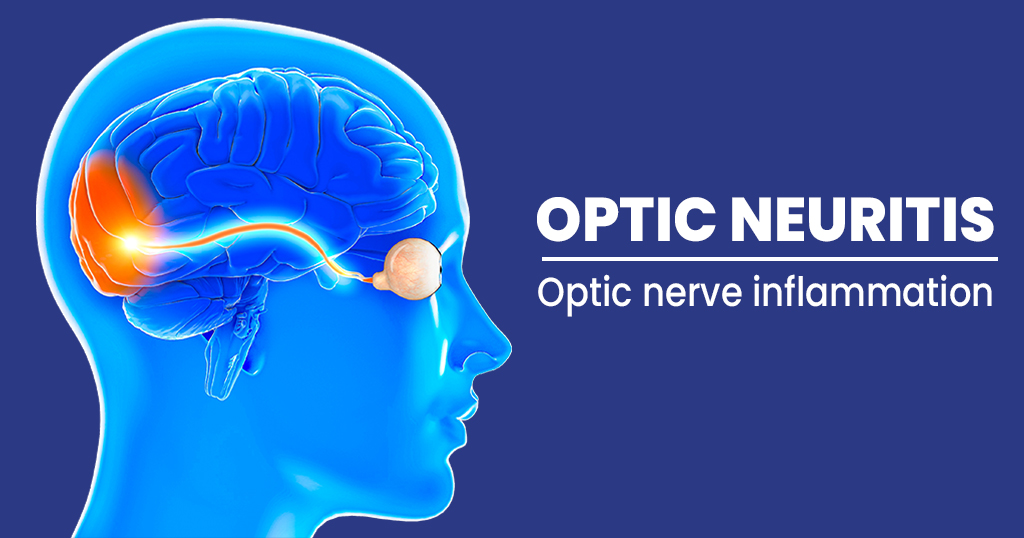
Optic Neuritis- Threat to vision loss
Interesting facts: -Usually monocular vision loss occurs. -Optic neuritis is the presenting feature of multiple sclerosis in 15-20% of the patients. -Females are more prone to develop the disease. -20 to 40 years of age group with acute/recurrent vision loss should be suspected with optic neuritis. Introduction It is an inflammatory, demyelinating condition that causes acute, usually monocular visual loss. When to suspect the disease? 1. Monocular vision loss (Vision loss typically develops over a period of hours to days, peaking within one to two weeks) 2. Eye pain that often worsens with eye movement, the onset of pain generally coincided with the visual acuity loss and improved along with it. Common visual symptoms and signs include: The acute phase includes: – Afferent pupillary defect – The visual field defects in optic neuritis is typically characterized as central scotoma – Papillitis with hyperemia and swelling of the disk, blurring of disk margins, and distended veins is seen in one-third of patients with optic neuritis. – Loss of color of vision out of proportion to the loss of visual acuity is specific to optic nerve pathology. – Photopsias(flickering or flashes of light) – Other signs of ocular inflammation can be observed by the ophthalmologist on fundoscopic or slit lamp examination. The Chronic phase includes: – Persistent visual loss – Color desaturation – Temporary exacerbations of visual problems – Optic atrophy How is the diagnosis of optic neuritis made? -Optic neuritis is clinical findings based on the history and examination findings. -An MRI should be done ( For confirmation of the diagnosis of acute demyelinating optic neuritis and important prognostic information regarding the risk of developing MS). -Lumbar puncture ( It is not an essential diagnostic test but should be considered in atypical cases in those with bilateral presentation and <15 years of age of individuals) – Antibody testing Is treatment available for optic neuritis? * Intravenous Corticosteroids are used in selected patients. Intravenous methylprednisolone 250mg four times a day for three days in acute phase of treatment. Some randomized trials have suggested that : High-dose Oral corticosteroids ( Methylprednisolone 500mg; prednisolone 1250mg) might have similar efficacy to intravenous agents in regard to vision outcomes and their small size precludes definitive conclusions. *Alternative therapy: Intravenous immune globulin and plasma exchange but these do not have established efficacy in the treatment of optic neuritis. Prognosis of the disease includes: Prognostic concerns in patients with optic neuritis are visual recovery, recurrence of optic neuritis, and risk of multiple sclerosis (MS). Recovery of vision — Without treatment, vision begins to improve after a few weeks. Improvement can continue over many months; 90 percent have 20/40 or better vision at one year. Some patients may have a more or less favorable prognosis: 1. Lower visual acuity at the time of presentation is associated with less complete recovery. 2. Longer lesions in the optic nerve, as demonstrated by magnetic resonance imaging (MRI), particularly those extending into the optic canal, are associated with poorer visual outcomes. approximately 20 percent will have a persistent functional visual impairment 3. Patients with MS may have a somewhat less favorable prognosis than those without Does the case of optic neuritis re-occur? – A randomized trial suggests that there was a 35% recurrence at 10 years, 14% in the original eye, 12% in the other eye, and 9% in both eyes.
Optic Neuritis- Threat to vision loss Read More »
Featured, Health, Newest